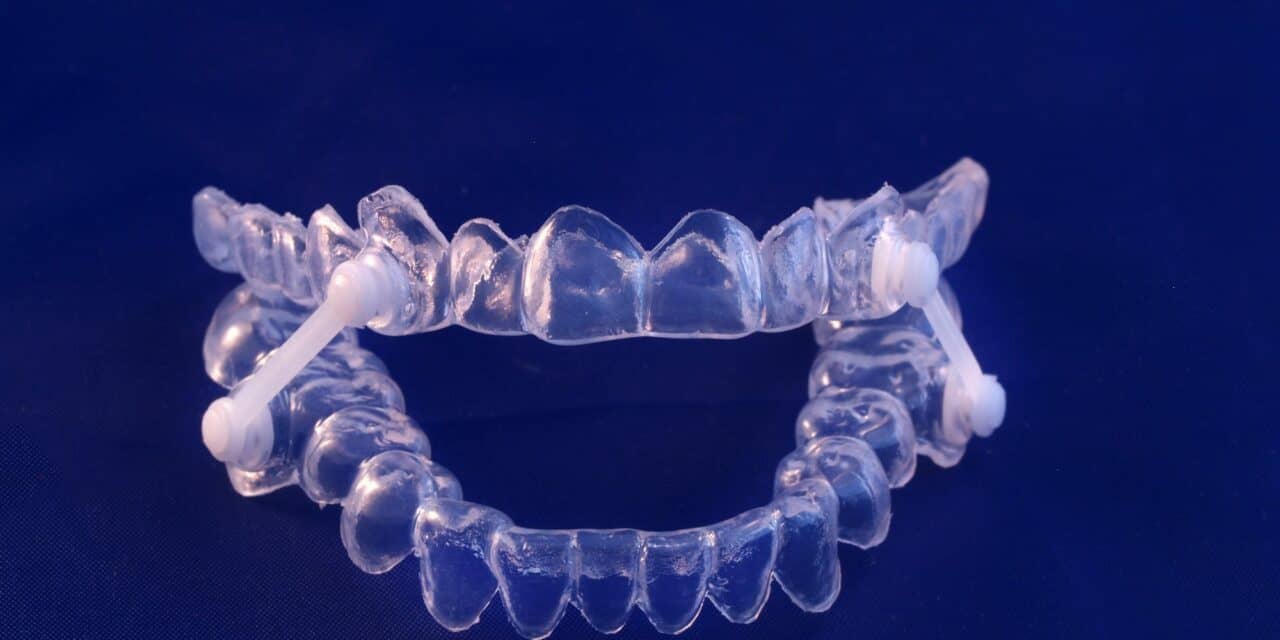
A new study found the therapy was comparable to CPAP in terms of change in the average 24-hour ambulatory mean blood pressure at six months.
CI’s Key Takeaways:
- A study comparing mandibular advancement device (MADs) (similar to a bite guard) to continuous positive airway pressure (CPAPs) devices found both equally effective in lowering blood pressure in patients with hypertension and obstructive sleep apnea over six months.
- Participants using the mandibular advancement device showed a larger average reduction in 24-hour ambulatory mean blood pressure and improved nighttime blood pressure compared to those using CPAP, with higher adherence rates noted among MAD users.
- The study, funded by the Singapore Ministry of Health and featured at the American College of Cardiology’s Annual Scientific Session, suggests that for patients who cannot tolerate CPAP, the mandibular advancement device could be a viable alternative for managing both sleep apnea and associated hypertension.
People with hypertension and obstructive sleep apnea were no less likely to see their blood pressure drop over six months if they used a mandibular advancement device (MAD) compared to a continuous positive airway pressure (CPAP) device, according to research featured at the American College of Cardiology’s Annual Scientific Session.
The study was simultaneously published online in the Journal of the American College of Cardiology at the time of presentation.
Hypertension, or high blood pressure, is a common risk factor for cardiovascular disease. People with obstructive sleep apnea experience frequent sleep interruptions due to the airway closing periodically during sleep. Since obstructive sleep apnea can cause or worsen hypertension, medical guidelines recommend the use of a CPAP machine to help keep airways open by delivering pressurized air through the mouth and nose.
MADs are designed to help keep the airway open by repositioning the lower jaw and moving the tongue forward. Previous studies have shown that CPAP devices outperform MADs in terms of apnea-hypopnea index, the standard metric used to measure sleep apnea severity. However, there is evidence that MADs may be better tolerated than CPAP, which some people find too uncomfortable or cumbersome for sustained use.
In this study, MADs were found non-inferior in terms of change in the average 24-hour ambulatory mean blood pressure at six months, and they resulted in a larger reduction across multiple secondary blood pressure parameters compared with CPAP. According to researchers, higher adherence among people assigned to use the MAD device could help explain the findings.
“Looking at the totality of evidence available in the literature, it is still reasonable to say that CPAP is the first-line treatment until we have more data on the MAD,” says Ronald Lee Chi-Hang, MD, professor of medicine at Yong Loo Lin School of Medicine, National University of Singapore, senior consultant in the department of cardiology at National University Heart Centre, Singapore, and one of the study authors, in a release. “However, for patients who truly cannot tolerate or accept using a CPAP, we should be more open-minded in looking for an alternative therapy such as a MAD, which based on our study, numerically had a better blood pressure reduction in patients compared with a CPAP.”
Study Details
For the study, 321 people with uncontrolled hypertension and high cardiovascular risk underwent a sleep study to determine whether they had obstructive sleep apnea. Of these, 220 people were found to have moderate to severe obstructive sleep apnea and were randomly assigned to receive a MAD or CPAP device.
Participants were instructed to use their assigned device for six months while sleeping to the degree that they could tolerate it. Both devices had built-in trackers that recorded use. At six months, people assigned to the MAD group experienced a drop in 24-hour ambulatory mean blood pressure that was 1.64 mmHg larger, on average, than those assigned to CPAP, meeting the threshold for non-inferiority and the trial’s primary endpoint.
Compared with the CPAP group, the MAD group also showed a larger between-group reduction in all ambulatory blood pressure measures, especially nighttime blood pressure when the devices were being used, and an increased proportion of patients achieving a systolic blood pressure below 120 mmHg by the end of the study. None of the participants experienced symptomatic hypotension.
The adherence data revealed that over half (56.5%) of those who were assigned to use the MAD used the device for six or more hours per night on average over the study period, while under one-quarter (23.2%) of those assigned to CPAP did so.
“The MAD patients simply used the device longer,” Chi-Hang says in a release. “That also might explain why the blood pressure reduction at nighttime, when the patients are actually using it, had a better reduction in the MAD arm.”
Adherence to the American Academy of Sleep Medicine’s recommendation of four or more hours of use in at least 70% of nights overall was similar between groups, with 69.4% of those in the MAD group and 64.3% of those in the CPAP group meeting this recommendation. Both groups saw a reduction in daytime sleepiness and the results showed no between-group differences in cardiovascular biomarkers.
Overall, researchers said the results underscore the importance of treating sleep apnea as part of a broader effort to control hypertension and reduce cardiovascular risk.
“People should be aware that over 400 million people globally have moderate-to-severe obstructive sleep apnea, and it is underdiagnosed and may be a contributing factor to their high blood pressure,” Chi-Hang says in a release. “Especially for patients whose blood pressure is hard to control or who have a lot of excessive daytime sleepiness, [it is important to] go see a physician about sleep apnea and get treated if necessary.”
Further Research Directions
Since the study was conducted in Singapore and most study participants were of East Asian descent, researchers said further studies in more diverse populations are necessary to determine whether the findings are generalizable to other racial and ethnic groups.
Chi-Hang also says that the timing of the study, which was conducted during travel lockdowns during the COVID-19 pandemic, may have influenced the results by increasing adherence.
The researchers plan to conduct further studies focused on comparing the impacts of the different types of devices on cognition.
The study was funded by the Singapore Ministry of Health.
Photo 115247277 © Jana Ščigelová | Dreamstime.com